Collectively — nurses Katie Osborn, Ingrid Crocco, Susan Fossum, and Maria Pedersen have volunteered with ReSurge International for 95 years, nearly a century between them. In that time, they’ve provided direct patient care, surgical support, nurse training, and more to underserved communities worldwide. But when COVID-19 shut down many aspects of the world in 2020, the nature of their volunteer work changed. Together, they adjusted to a new normal and transitioned to delivering virtual training to nurses across the globe.

This year, they met in Amsterdam to share a presentation highlighting their unique experience at the 2023 International Collaboration of PeriAnaesthesia Nurses (ICPAN). Their session, titled “Perioperative Nursing Education Reimagined,” shared the struggles and successes of virtual nursing education— shining a light on the evolving hybrid model of training ReSurge implements today.

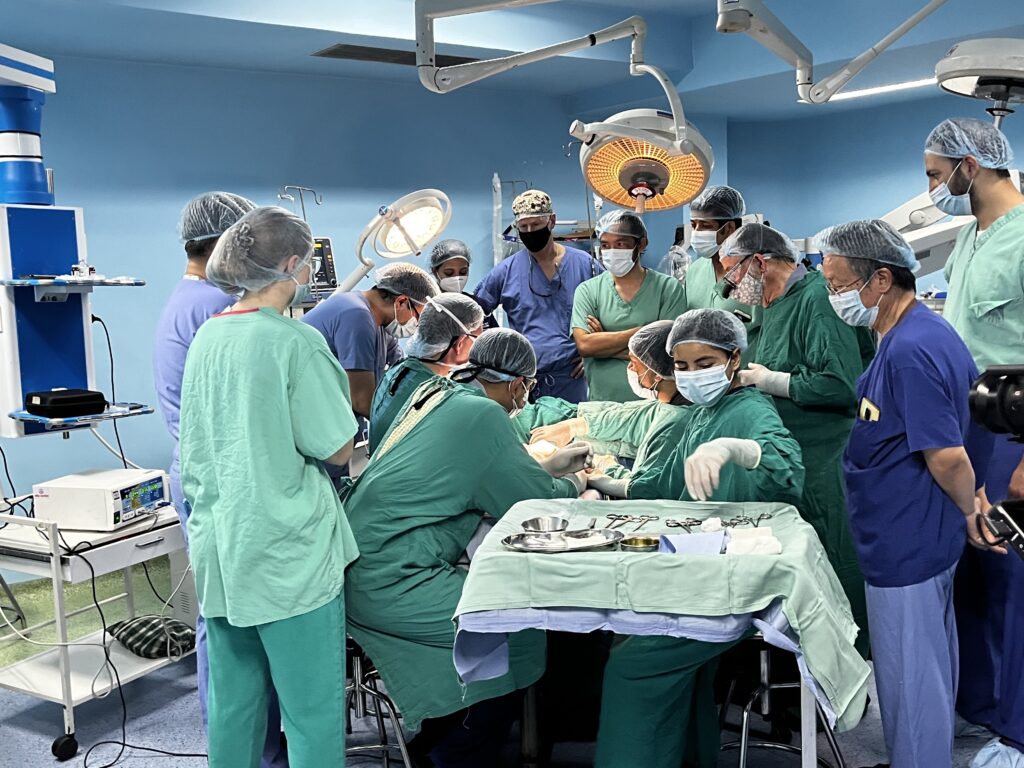
Before the pandemic, ReSurge volunteers provided in-person nurse education during site visits.
“We were assigned and participated in patient care, educating at the bedside in small groups,” Ingrid shared, describing the ReSurge trips she served on before the pandemic.
With their invaluable work under threat in the face of COVID-19, Katie, Ingrid, Susan, and Maria adjusted to a new teaching method – shifting to virtual education. The transition was challenging.
“One issue was access,” shared Susan. “Host countries needed access to rooms that had the space, Wifi, and bandwidth to engage in a virtual class.”
Of course, access would not be the only issue – volunteers also had to find new ways to evaluate local capacity to determine which lessons were needed and to measure the impact of their training. As a result, local contacts were key in these circumstances – an early sign that communication would play a pivotal role in delivering effective virtual nursing education.
As everyone involved adjusted to the new training format, the volunteer nurse educators found some benefits in virtual education. One unexpected impact was that, as nurses had to leave patient bedsides to receive training in a designated area, the education was more focused.
“The biggest benefit is that it was protected time,” said Ingrid. “There were no distractions for the nurses in our classes.”
Katie also noted increased participation and communication in the training, especially in one particular virtual class delivered to nurses in Uganda.
“We began the classes with about 7-10 nurses. Word spread and more people began attending. One particular class had 41 attendees, including medical and nursing staff.”


Not only did the classes grow in size – they expanded to include other members of the medical team and increased communication between nurses and doctors.
“After presenting the content, there were many questions that ended up in a general discussion between the nurses and the doctors. It was gratifying because, typically, there wasn’t a great deal of interprofessional communication,” shared Katie.
Eventually, in-person education trips resumed. However, the nurses found value in holding onto the best parts of virtual teaching
“Once we were traveling again, ReSurge went to a hybrid model. We were able to combine lectures, precepting, and hands-on practice,” Ingrid explained. “There was time carved out to have a more formal teaching followed by application afterward. If done correctly, this is a very successful and sustainable approach to teaching.”
Katie, Ingrid, Susan, and Maria shared that they’re still trying to strike the right balance for hybrid training.

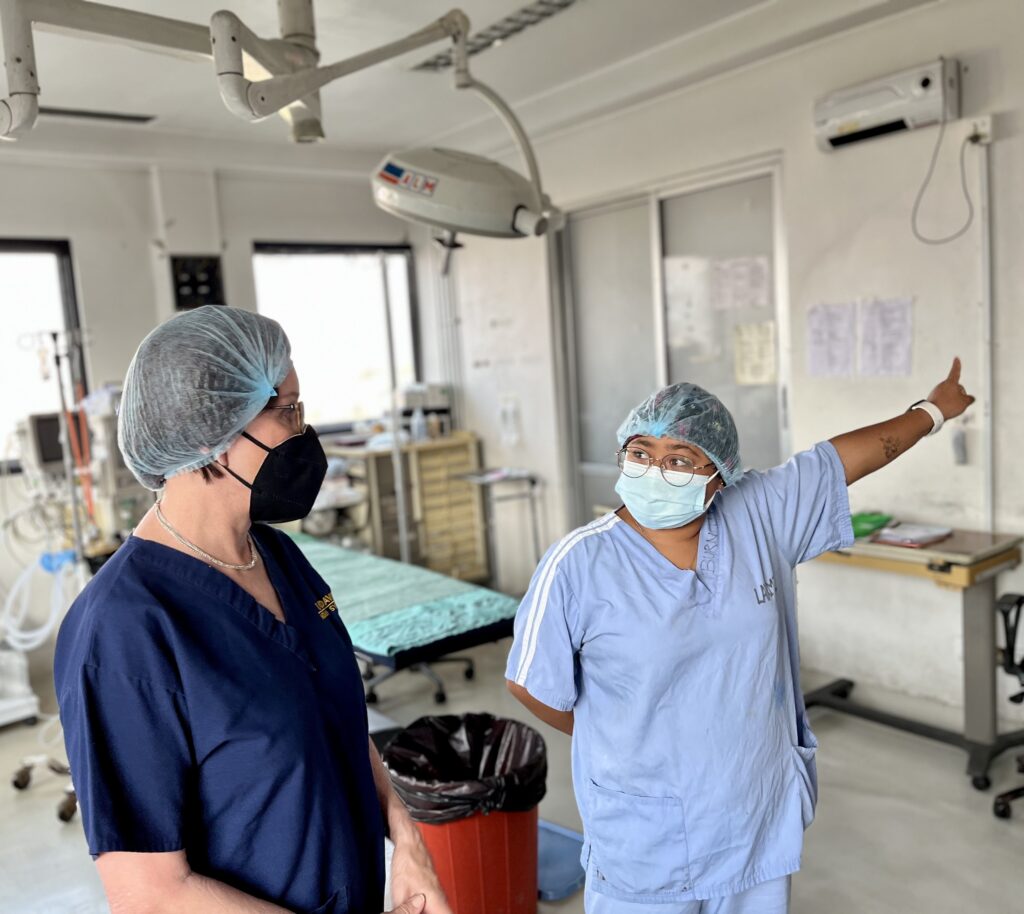
“The verdict is still out, and there’s definitely room for improvements,” Maria shared when asked about the hybrid training model. However, the team agreed that they hope to hold on to the best of both worlds when it comes to hybrid training – including the increased communication required by virtual classes.
“For years, we would go, present six topics, then return home. We’d never hear a word after that – we just didn’t communicate,” Katie explained. “With ReSurge’s new model, we’re doing pre-trip and post trip calls. I think it’s enriched the whole educational experience at the sites.”
ICPAN attendees were very engaged in the volunteers’ presentation – especially one nurse who praised two assessment tools that Katie, Ingrid, Susan, and Maria designed together. Called the Adult Patient Assessment Record and Pediatric Patient Assessment Record, the tools outline the process of assessing patient status, nursing interventions for abnormal assessment findings, and the need to report critical information to doctors. During the presentation, a nurse from the Philippines was inspired by the tools’ emphasis on interprofessional communication.


“He was most impressed with the guides’ last column, which states when and what to communicate with the physicians,” Katie shared. “He said he attended nursing school in the Philippines, where they were taught not to speak to the physicians. He believed it is vital for nurses in the developing world to use critical thinking skills to assess patients and understand that patient safety depends on communicating with physicians.”
The volunteers plan to introduce the assessment tools at all Resurge sites. Nurses in Uganda, Mozambique, and Nepal have already been taught how to use these tools through virtual education followed by in-person reinforcement during hybrid trips. The volunteers hope this implementation leads to increased communication between nurses and doctors, resulting in improved patient outcomes.

Upon their return from ICPAN, all four nurses expressed hope for the future of ReSurge training. Despite continued challenges in their work, including nurse turnover, they came home re-energized.
“It was really satisfying to connect with our colleagues,” Maria shared regarding ICPAN. “The last few years made it hard to feel a connection with your organization. This helped me stay inspired.”
The work of ReSurge volunteers like Katie, Ingrid, Susan, and Maria changes lives around the world. If you are interested in volunteering, apply on the ReSurge website.









